Cancer
-
Aspirin, taken by around 29 million Americans daily, has increasingly been linked to inhibiting the growth of certain cancers – but we didn't quite know how. Now, scientists have uncovered how it helps the immune system see and kill cancer cells.
-
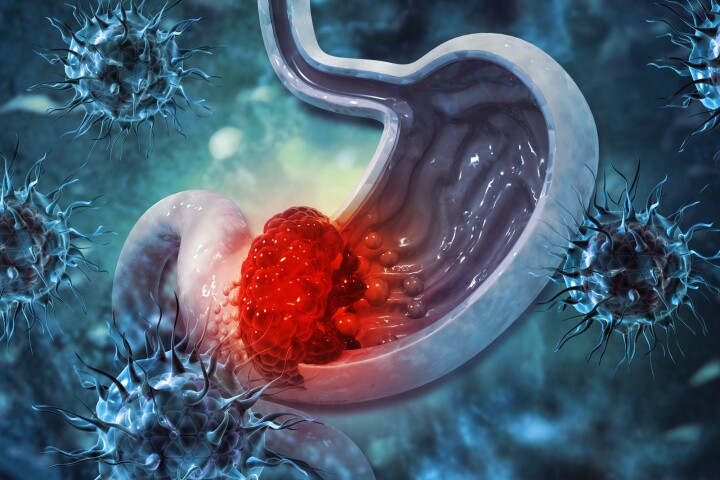
A common, usually harmless bacteria has been found to have a significant role in causing stomach cancer. Researchers identified the bacteria’s mechanism of action, opening the door to developing therapeutics that prevent it triggering cancer growth.
-
Researchers have identified two genetic markers that may explain the link between eating red and processed meat and bowel cancer. Understanding the disease process and the genes underlying it can help develop better prevention strategies.
-
If someone you know has gone through chemotherapy, you might be familiar with the side effect 'chemo brain.' Scientists have now demonstrated a simple way to protect brain cells from damage using flashing lights and sounds at a certain frequency.
-
The biggest tragedy of pet ownership is that they just don’t live long enough. Thankfully scientists are working on that, with a new cancer vaccine for dogs that almost doubles their survival rates in the face of certain types of the disease.
-
In a true public service, potato scientists have flicked the 'off' switch on a genetic mechanism that causes cold-stored taters to produce carcinogenic acrylamide when cooked. It means that one of the world's greatest food groups could be made healthier.
-
The 102-year-old tuberculosis vaccine shrank liver cancer tumors in mice, which suggests it may be replicated in a human trial. If this was the case, the vaccine might prove successful in tackling this notoriously hard-to-treat cancer.
-
A radioactive form of fructose, a natural sugar found in fruit, can illuminate cancer and inflammation in medical scans. This approach has the potential to make diseases easier to spot than current techniques, leading to better early detection.
-
February 11 marks International Day of Women and Girls in Science. The day celebrates both the work of women across vast scientific disciplines, but also recognizes ongoing gender-based challenges. Here, we pay tribute to 11 stars of STEM today.
-
Researchers created model tumors using the tissues of patients with bowel cancer and used them to predict how the disease will respond to specific drugs with 83% accuracy. The pioneering approach could ensure patients get the most effective treatment.
-
In the hunt for cancer cures, researchers work with structures known as tumor spheroids. A new method of producing these structures has emerged using simple parts, which could lead to the cheap, reliable generation of these valuable research tools.
-
No matter how important something is, too much of anything is bad for you. Scientists have now put that principle to work to kill cancer, with a new drug that causes calcium to build up and choke the tumor to death.
Load More