Melanoma is the deadliest of skin cancers. In 2010 U.S. doctors diagnosed nearly 115,000 new cases of melanoma, with nearly 8,700 resulting in death. Scientists at Duke University have developed a new laser-based tool designed to identify malignant melanomas sooner, without the expense of false diagnosis and unnecessary surgery.
The new technique involves using two low-energy lasers to probe suspect moles. The redistribution of energy is examined to identify microscopic areas of varying skin pigment. In the study, forty-two skin samples were probed with the double laser tool, highlighting higher levels of a skin pigment known as eumelanin in melanomas. Using this higher presence of eumelanin as the indicator, the team was able to positively identify all eleven samples of melanoma in the study.
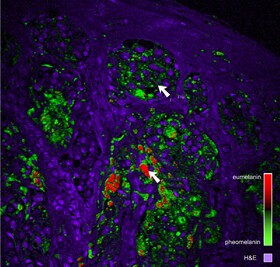
The trial will continue using thousands of archived skin slices as tests. The team also hope the technique will correctly identify samples from moles that eventually became cancerous.
"For the first time, scientists have the ability to identify substantial chemical differences between cancerous and healthy skin tissues," said Thomas Matthews, a Duke graduate student who helped to develop the new microscopy technique.
Currently the laser can only be used with tissue on slides, but Matthews is also trying to develop a technique to image skin cancers in situ. However this would be a much more expensive device and they do not expect it to be ready for several years.
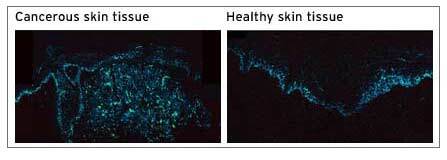
Although melanoma is the fifth and sixth most common cancer in males and females respectively, current diagnosis by biopsy is expensive and often misleading. The present method involves a light and a magnifying glass, or a tissue biopsy. Suspicious skin cells are removed and examined by a pathologist under a microscope to spot signs of disease. In an age of technology a lens and a light could be seen as archaic, especially when it is only 85 percent accurate at best, and tissue biopsy is not much better.
According to the 2010 study published in the Journal of American Academy of Dermatology, pathologists would disagree on the diagnosis of sampled cells in 14 percent of biopsy diagnoses, which follows that 214,000 to 643,000 diagnosed melanoma cases each year could be open to argument. "Even if the technique proves, on a large scale, to be 50 percent more accurate than a biopsy, it would prevent about 100,000 false melanoma diagnoses," said Warren S. Warren, director of Duke's Center for Molecular and Biomolecular Imaging and a chemistry professor.
The lasers required for creating the tool are already commercially available and it costs around US$100,000 to retro-fit them to the usual microscopes used by pathologists.
While the cost of the equipment may sound high, the saving to healthcare overall must be considered. The typical response to any questionable melanoma is "when in doubt, cut it out" but in fact many are benign and do not need removal. Furthermore additional healthy skin is often removed in a pre-emptive strike, and beyond first and second tissue biopsies costing thousands of dollars, additional treatments can include expensive chemotherapy and surgical lymph node removal.
The results from Duke University's study appeared in the February 23 Science Translational Medicine.





